Your Strategic Partner in the Operational Success of Every Project
From design to delivery, we help firms reduce costs, improve efficiency, and scale confidently.
Our Services
We partner with firms to eliminate delays, reduce overhead, and scale with confidence. Explore our core offerings below.
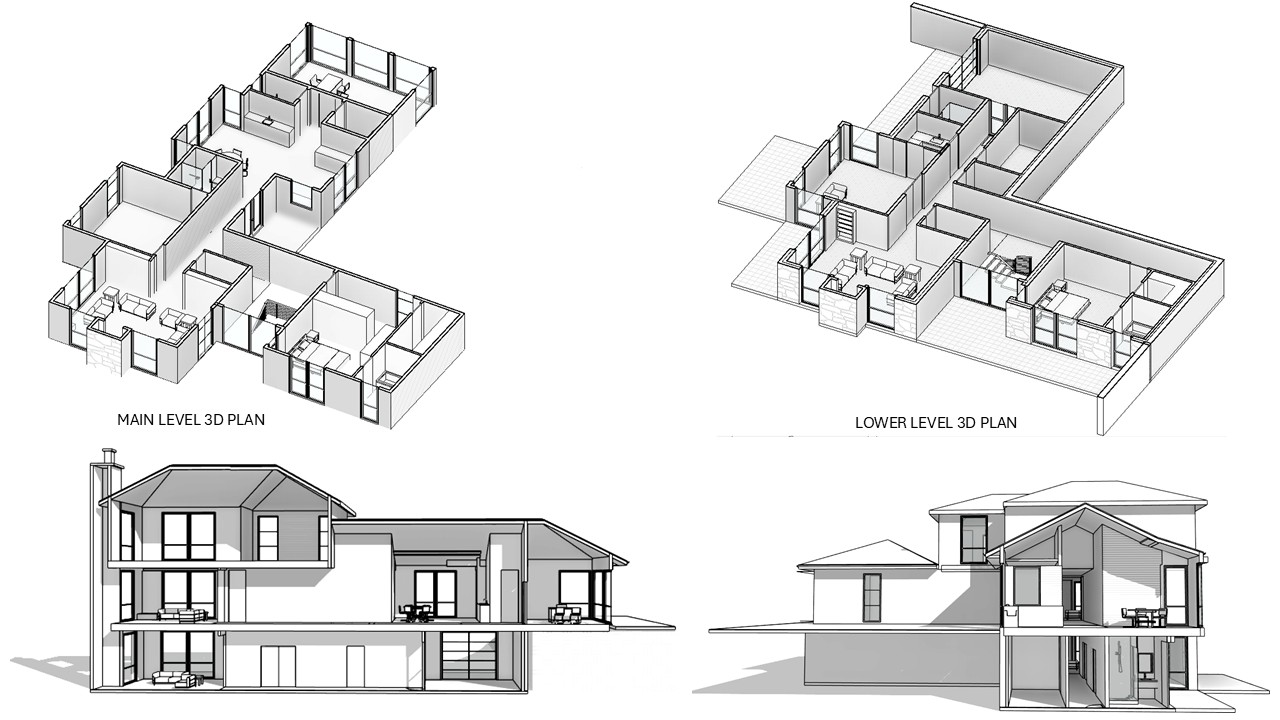
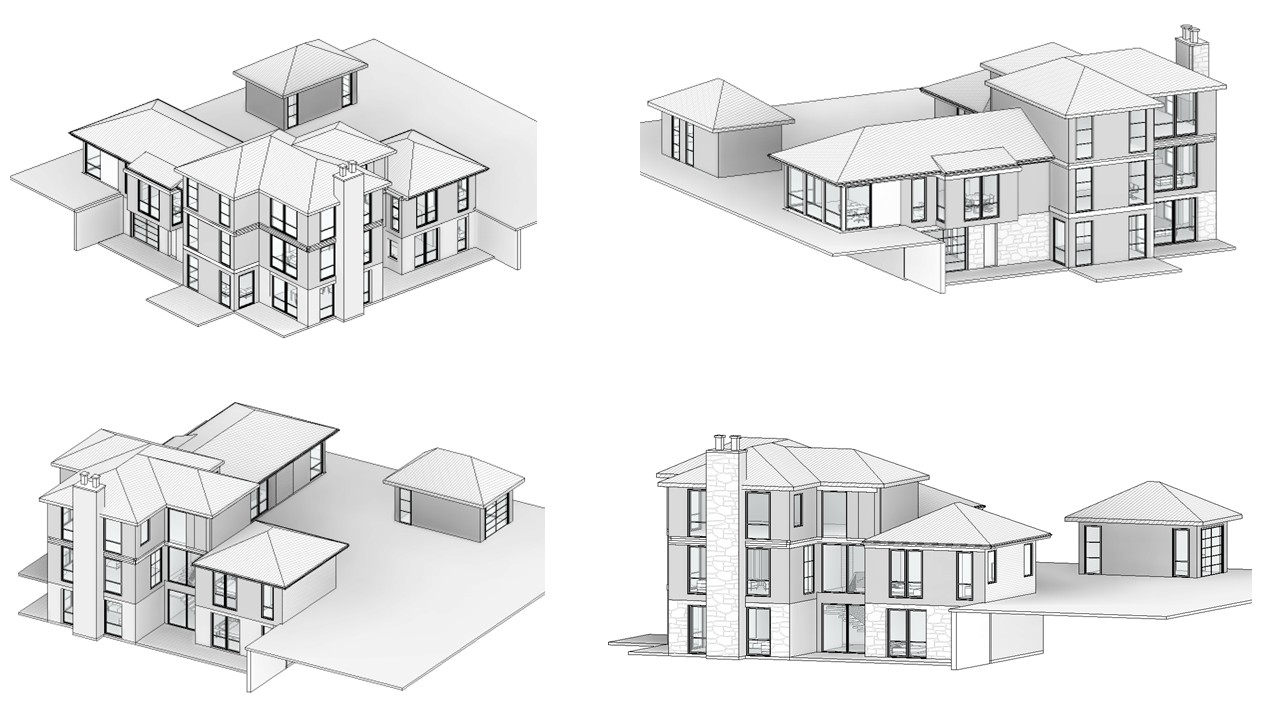
Architecture, Engineering, and Construction (AEC)
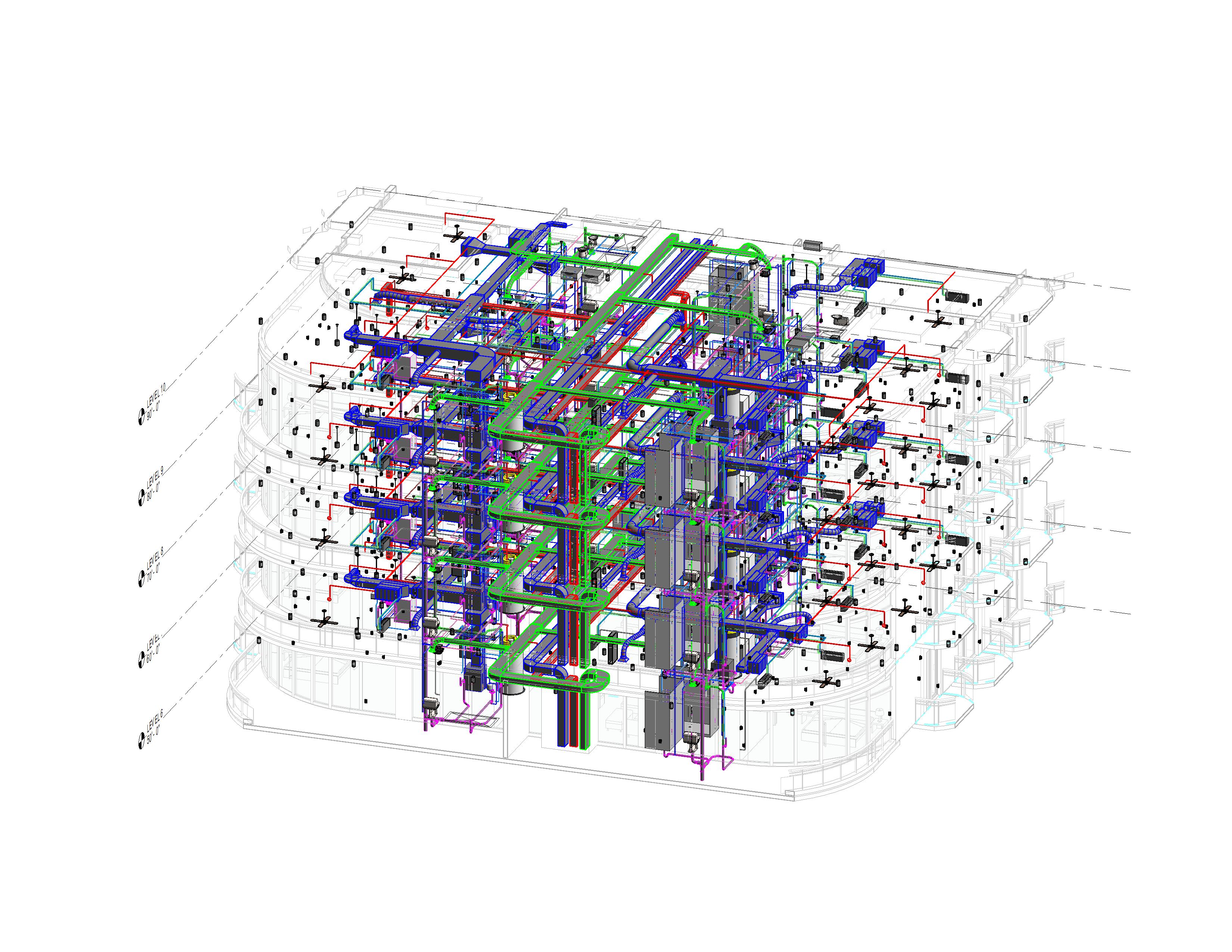
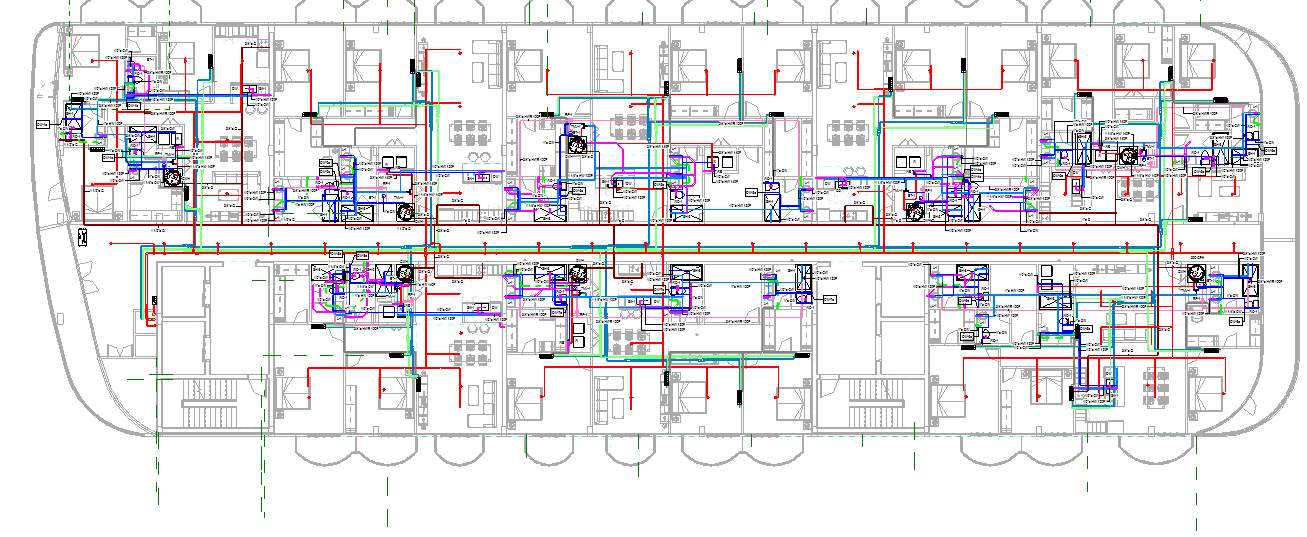
Comprehensive BIM, CAD, and MEP support including clash detection, shop drawings, construction documentation, permit-ready drawings, scan-to-BIM, and design development across architectural, structural, and MEP disciplines.
Engineering Solutions
End-to-end engineering support including design engineering, CAD modeling, simulation (FEA/CFD), prototyping, product lifecycle management (PLM), and manufacturing-ready design to accelerate innovation and time-to-market.
AI & Technology
Full-cycle IT support including application development, CAD automation, UI/UX design, system integration, RPA (robotic process automation), AI/ML solutions, dashboard development, data analytics, and reporting to drive smarter, data-informed decisions.
Rendering & Animation
High-quality 2D/3D visualization including photorealistic renderings, product animations, explainer videos, walkthroughs, and AR/VR-ready content for training, marketing, and stakeholder presentations.
Logistics
Back-office logistics and freight support including freight bill processing, audit and payment, customs documentation, shipment tracking, carrier onboarding, insurance verification, and import/export documentation management.

About Our Company
Accuracy, Competency, and Teamwork
Our commitment to accuracy has earned recognition from top-tier clients who rank us among the most precise partners in the industry. We foster competency through continuous learning—supported by our Sona College. And we believe teamwork is the foundation of success, enabling seamless collaboration across teams and with every client we serve.
Our services empower organizations of all sizes to reach exceptional outcomes. We work across industries to streamline operations, reduce costs, and accelerate growth by aligning our solutions with each client's most critical goals.
How We Solve Real Problems
Explore how leading organizations overcome complex challenges through real-world solutions. Our curated Case Studies and White Papers highlight measurable results, client success stories, and actionable insights—covering everything from BIM strategy and CAD automation to process optimization and digital transformation.
Stay ahead of industry shifts with expert guidance, trend analysis, and proven frameworks—designed to inform decision-making and inspire innovation.
Our Work
See how we deliver measurable impact across industries through smart, scalable solutions.

Challenges & Opportunities in Aftermarket Components Engineering
The global automotive aftermarket is faced with multiple challenges ranging from varied expectations and unique customer requirements, to disruptive technologies.
More Details
Utilizing RPA to Streamline Logistics Template Classification
The client is a global provider of third-party transportation information services. They offer comprehensive freight payment, auditing, accounting and reporting services to their c...
More Details
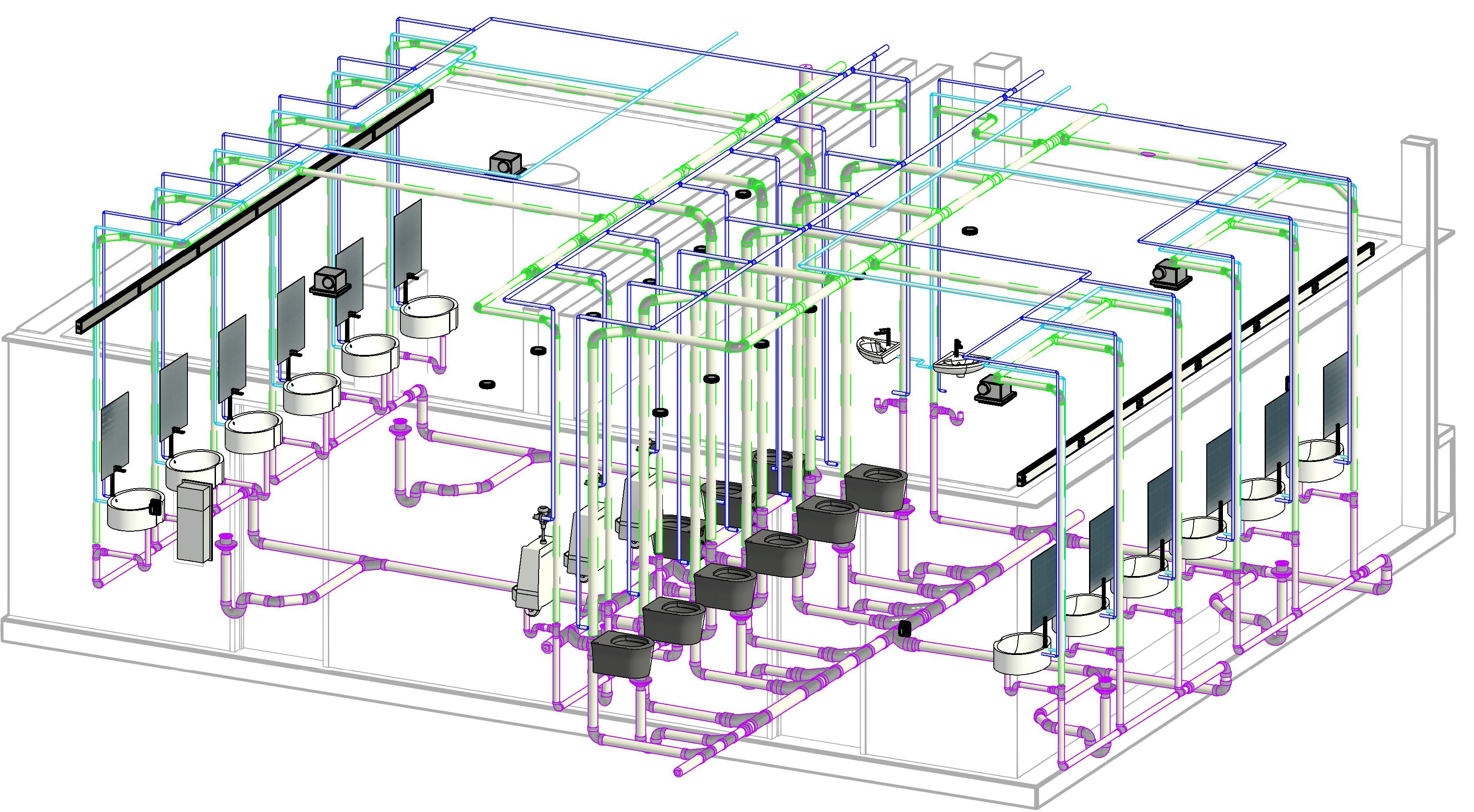
Point Cloud Project (MEP)
Project Brief: This stadium project, based in USA, involved modeling MEP services from point cloud data. The client provided ReCap files along with architectural and structural Rev...
More DetailsGet in Touch
We're here to help. Fill out the form and a member of our team will be in touch shortly to learn more about your needs and how we can support you.
Contact Information
info@veetechnologies.comUSA: (929) 730-2544
India:
080 2308 5600
News & Events
Industry Leading Expertise With a Commitment to Our Clients
What Our Clients Say
Trusted by Over 1,500 Clients Worldwide
5K+
global team members
Supporting operations and innovation across time zones.
10K+
satisfied clients served
Including Fortune 500s and fast-growing enterprises.
10
offices in 7 counties worldwide
Expanding reach while staying locally responsive.
Ready To Start?
Connect with our experts for tailored solutions to your most urgent business challenges.
Get in TouchLooking For a Job?
Ready to grow your career? Join a global team that values innovation, impact, and individual growth.
View Open Role